When the news of Monkeypox first spread across national headlines, American media began to follow the same homophobic patterns it first made with HIV/AIDS. The belief that HIV/AIDS is a disease limited to the LGBTQ+ community was compiled into the plethora of disparities and roadblocks that negatively impact Black Americans' health outcomes in regards to HIV/AIDS.
Rather than the focus being on health, the focus was on proving you were straight. When the news of Magic Johnson having HIV/AIDS broke, the conversation was surrounded in homophobia rather than being about decreasing transmission for the overall wellness of Black Americans. As a result, taking measures to prevent HIV/AIDS was seen as an admission to being Queer rather than practicing safe sex. This stigmatization cannot be brought into the reaction toward Monkeypox. Black Americans already tend to have negative health outcomes from other epidemics and stigmatizing a disease will only worsen these outcomes.
Currently, one of the most effective ways to prevent Monkeypox is to be vaccinated. Unfortunately, Black Americans have a pattern of having low vaccination rates. Not for just no reason though, I’m sure we’re all familiar with the Tuskegee Syphilis Experiment that has caused countless Black Americans to have difficulty trusting in our healthcare system. And while fears and apprehension are incredibly valid feelings to have, these same feelings are factors that directly affect the survival rate of Black Americans during pandemics.
These disparities were incredibly prevalent during the peak of COVID-19. According to The Covid Tracking Project, Black Americans died at a rate 1.4 times the rate of White Americans. And according to the CDC Black Americans are also less likely to be vaccinated against COVID-19. Now of course there’s an overwhelming number of factors that also impact these statistics. Health disparities such as access to vaccine clinics, inability to take off of work to get the vaccine (and in many cases, the need a day or two off to recover from it), and discrimination from healthcare providers are just some of the reasons that vaccination rates are so low, and deaths are so high.
But the painful truth is that there is not much we can do individually to change these disparities. Yes, over time we can change them, but pandemics don’t wait for us to fix inequitable systems. The best thing we can do at this moment is to work on disparities we can change right now. As I stated earlier, distrust in our healthcare system is incredibly valid to feel. Educating ourselves to make well-informed decisions on whether or not to vaccinate is the best way to take control of our health and feel assured in our decisions. We need to do our best to destigmatize and encourage informed health decisions in our approach to combating Monkeypox.
Where should I start my research?
Information on what vaccines are out there, when vaccination should occur, who can get infected, and which are FDA-approved:
What does it mean to be FDA approved? How does this affect you?
Approval takes years to come about. There are many steps to approval including pre-clinical testing, Investigational New Drug application for clinical trial, and clinical trials (meaning trials on humans) that are broken into three phases (small group, large group + dosage variation, and finally large group + long term efficiency and side effect study), lastly medical, chemistry, and biology experts will weigh in on the safety and efficacy. This long process serves as reassurance that questions regarding side effects, long term usage, and effectiveness of vaccines on large populations were all thought about and answered.
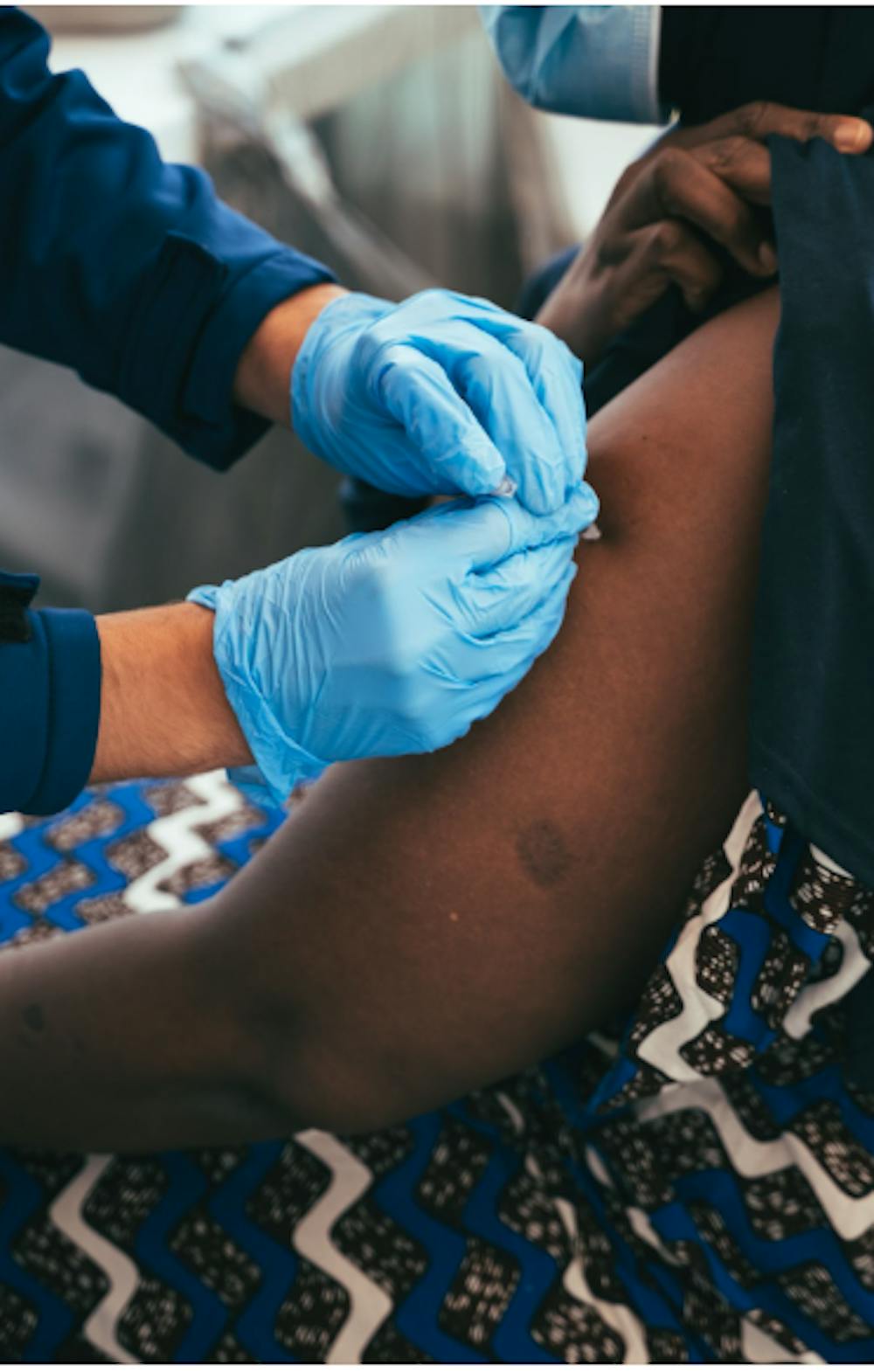
Those who get vaccinated before exposure to Monkeypox are much more likely to prevent disease according to the CDC However vaccination can still occur after exposure to Monkeypox and should be done within four days post-exposure. The vaccine is usually administered in the forearm but there are also options to have the vaccine done in a more discreet location if privacy fears are a barrier to getting vaccinated.
To find out more about some of the clinics nearby, I interviewed an AU student, (who prefers to remain anonymous) that visited the I Street clinic for his first vaccine:
“The process was extremely easy; I was pretty much in and out... Then I was called back by a vaccine administrator who was a very kind woman…and I sat down and was given the vaccine, I needed to sit down for 15 minutes afterward to make sure everything was okay and was told to come back 28 days later. I honestly haven’t had a vaccine experience as pleasant as this one.”
Dealing with a new epidemic is stressful and overwhelming. It seems like every few months there’s a new thing we should be vaccinated from, but it’s important that we take the steps needed to ensure our overall wellness and protect our communities from mass spread.
Wondering where you can get vaccinated?
Below are three vaccination clinics in the D.C area that are now available for walk-in vaccinations:
1900 I Street NW; Hours: Sunday-Friday 12-8 p.m.
7530 Georgia Avenue NW; Hours: Sunday-Friday 12-8 p.m.
3640 Martin Luther King Jr. Avenue SE; Hours: Monday-Saturday 12-8 p.m.
If you still have any lingering questions, please call the Washington Health Institute at 202-525-5175 for any answer you may need. If you feel that you may have been exposed to monkeypox or are experiencing symptoms, the Student Health Center recommends contacting them as soon as possible to be seen. You can visit MPV (formerly known as Monkeypox) Information and FAQ | American University, Washington, DC for more information.